How to Use Flexible Intramedullary Nails for Effective Surgery?
Flexible Intramedullary Nails are gaining attention in orthopedic surgery. Dr. Emily Carter, a renowned orthopedic surgeon, stated, "These nails offer unparalleled stability and flexibility." Their unique design facilitates better alignment in fractured bones.
Surgeons now prefer this method for various long bone fractures. However, using Flexible Intramedullary Nails is not without challenges. Proper technique is crucial for successful outcomes. Surgeons need extensive training to master the insertion process.
Despite the advantages, there can be complications. Nail bending or improper placement may occur. Surgeons must remain vigilant and attentive to detail. Continuous learning and adaptation are key in this evolving field. Emphasizing the balance between innovation and precision will enhance surgical success.
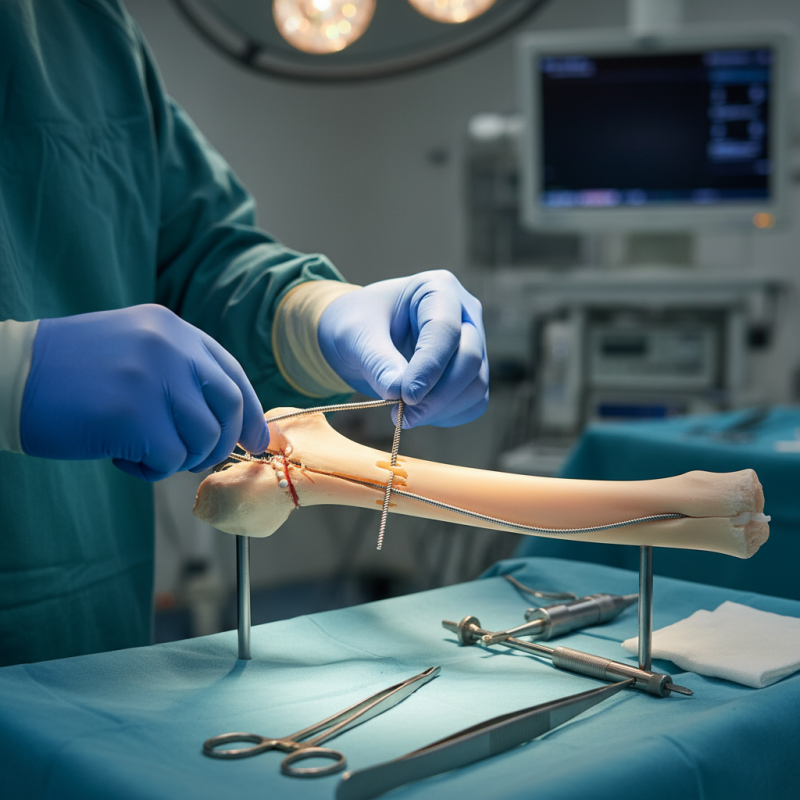
Understanding Flexible Intramedullary Nails: An Overview of Surgical Use
Flexible intramedullary nails (IM nails) play a crucial role in orthopedic surgeries. They are especially valuable for long bone fractures in children and adults. According to recent studies, flexible nails can reduce surgery time by 30% compared to traditional methods. This efficiency is vital for patient outcomes.
Surgeons appreciate the versatility of flexible IM nails. They can adapt to different bone geometries and fracture patterns. Notably, pediatric applications have shown a 90% success rate in aligning femoral fractures. However, challenges remain. The risk of malrotation or improper alignment can still occur. Surgeons must carefully plan each case.
Training for using flexible IM nails is essential. Some studies suggest that less experienced surgeons may face complications. Ongoing education and hands-on practice are necessary to enhance skills. An interactive training module can improve surgical outcomes significantly. Maintaining a focus on technique is paramount in using these innovative devices effectively.
Indications for Flexible Intramedullary Nails in Orthopedic Surgery
Flexible intramedullary nails offer a versatile solution for various orthopedic conditions. They are particularly indicated for the stabilization of certain types of fractures. This method is commonly used for pediatric fractures, especially in long bones. Children tend to heal quickly, requiring minimal invasive procedures.
These nails allow for better alignment and reduced risk of complications. However, proper case selection is crucial. Not all fractures are suitable for this technique. Misjudgments in fracture types can lead to complications, including malunion or nonunion. Surgeons must assess each case carefully, considering factors like fracture location and patient age.
Additionally, using flexible nails necessitates a good understanding of biomechanics. A surgeon may encounter challenges when dealing with complex fractures. Adjusting the nail's positioning can sometimes be tricky. These factors should encourage orthopedic professionals to reflect on their techniques continuously and remain open to learning.
Step-by-Step Surgical Procedure for Inserting Flexible Intramedullary Nails
When performing surgery with flexible intramedullary nails, careful preparation is crucial. Begin by positioning the patient correctly on the operating table. Use fluoroscopy to obtain images of the bone. This will help in planning the nail insertion with precision.
Next, prepare the surgical site by cleaning and draping. A small incision is typically made at the entry point. The entry point must be aligned with the medullary canal for optimal insertion. The use of a reamer may be necessary to facilitate the process. Be cautious; improper alignment can lead to complications.
Once the nail is inserted, verify its position using imaging. Ensure that the nail spans the fracture site adequately. Pay attention to any signs of difficulty during insertion. It's essential to reflect on the method and adapt if necessary. The last step involves securing the nail in place and closing the incision carefully. After surgery, monitor for potential complications, as they can greatly affect recovery.
How to Use Flexible Intramedullary Nails for Effective Surgery
| Step | Description | Tools Required | Expected Outcome |
|---|---|---|---|
| 1 | Patient Preparation and Anesthesia | Anesthesia kit, sterile drapes | Patient stabilized and ready for surgery |
| 2 | Incision and Exposure of the Medullary Canal | Scalpel, scissors, retractors | Access to the medullary canal achieved |
| 3 | Nail Preparation and Measurement | Flexible intramedullary nails, measuring tools | Properly sized nail for insertion |
| 4 | Insertion of the Intramedullary Nail | Insertion tool, fluoroscopy for guidance | Nail correctly positioned in the canal |
| 5 | Finalizing the Procedure and Closure | Sutures, dressing materials | Surgical site closed and secured |
Benefits and Complications Associated with Flexible Intramedullary Nails
Flexible intramedullary nails are becoming popular in orthopedic surgeries. They provide several benefits, particularly for pediatric and minimally invasive procedures. One major advantage is their ability to allow for stable fixation. This enhances the healing process in fractures, significantly reducing recovery times. Surgeons appreciate their versatility and ease of application. However, not all outcomes are perfect.
Despite these benefits, complications can arise. Misalignment may occur during insertion, leading to poor healing. Moreover, infection risk remains a concern. Surgeons must always evaluate the patient’s individual situation. Balancing the benefits and potential complications is crucial for optimal results. In some cases, patients may experience discomfort or require additional surgery.
Surgeons are advised to remain vigilant. Continuous training and assessment of techniques can minimize risks. Open communication with patients is also necessary. They should be informed about potential drawbacks. Patients may be hesitant after hearing about complications. Ultimately, understanding both the advantages and challenges is key for effective surgical outcomes with flexible intramedullary nails.
Usage of Flexible Intramedullary Nails in Surgery: Benefits and Complications
Postoperative Care and Rehabilitation Strategies After Nail Surgery
Postoperative care is crucial after intramedullary nail surgery. Effective rehabilitation can significantly influence the outcome. Studies indicate that about 30% of patients experience complications related to improper postoperative care. Pain management, swelling reduction, and mobility restoration are key focus areas during this period.
Physical therapy often starts within weeks. Gentle exercises can enhance blood circulation and prevent stiffness. However, not all patients follow through with therapy. Adherence rates can be as low as 50%. This can delay recovery. Regular follow-ups are essential to monitor healing progress. Providers should encourage communication about concerns regarding pain or mobility.
Nutrition also plays a role in recovery. A diet rich in calcium and vitamin D supports bone healing. Yet, many patients neglect their nutritional needs post-surgery. This could impact bone density and overall recovery. Balancing care strategies with emotional support may be beneficial, as psychological factors can hinder rehabilitation. Addressing these elements is paramount for a successful recovery journey.